Vol. 2, No. 6, February 1979
ERRORS
Too frequently a correct measurement of the short leg in the supine position is not accurately obtained. Supine leg checking requires that the practitioner knows the reference points, and is capable of visualizing them. Unless mental images are formed by the practitioner of the points of reference, he can commit errors that render his efforts ineffectual. Checking for leg length deficiency is a highly subjective process, and too often ends as a matter of opinion, not of fact.
The orientation planes of the patient and the practitioner provide the most accurate guide. If correctly used, these planes determine the required degree of accuracy essential in making a correct determination of the amount of leg deficiency. The patient’s head, shoulders, spine, pelvis, knees, and feet can, for example, be aligned directly to the patient’s mid sagittal plane, which can be depicted by drawing a line, or it can be visualized.
ANOMALIES
The short leg, caused from a pathological, congenital, or other anomalous reason will be measured differently. The amount of leg deficiency may be recorded in these cases with considerable accuracy if the C1 subluxation is first corrected to normal and verified by post-x-rays and ANATOMETER recordings of previously registered bodily distortions. Corrections, or normalization of the misalignment factors of the C1 subluxation, removes the subluxation-induced shortness, leaving only the shortness caused by anomaly. Shoe lifts may then be used as body-balancing devices to correct the deficiency caused by anomaly. The subluxation-induced deficiency should be corrected only by the adjustment.
The difference will have to be established between the two causes of leg disparity, because the body is precisely balanced in the normal state and quite subject to structural adaption to the short leg. The use of shoe lifts to equalize the subluxation induced short leg is an erroneous procedure because they interfere with normal structural adaptation of the spinal column which results from the correction of the subluxation.
IMPORTANCE OF LEG-CHECKING
The existence of a leg deficiency in the absence of anomalous reasons is a positive indicator of imbalance in the central nervous system (CNS), and of spastic contracture of the extensor, or anti-gravity, musculature, and is caused by the C1 subluxation. The C1 subluxation, detrimentally affects the CNS, the reticular formation of the brain stem, and causes the muscular contracture. Bodily distortions, pelvic obliquity, and the short leg result. Thus, the presence of the short leg is symptomatic of a subluxation of C1. A C1 subluxation, therefore, is a stress-producer of the body.
Not only does the short-leg indicate the presence of nervous imbalance in the CNS, but the amount of shortness can indicate the degree of neurological imbalance. The shorter the leg, the greater the degree of detriment, generally speaking. It does not, however, indicate the severity of the excursions of the subluxation into the planes of motion. Of importance to the practitioner is that the variance in leg length seen on different office visits suggests different things and may be of aid to him in charting his course of action on that visit: how much to adjust, if his patient is making progress, and so on.
Leg length varies for several reasons, and careful records of the amount of leg shortness should be recorded on each visit. If, of course, the legs are equal, no nerve imbalance is indicated; therefore, no adjustment is required. This fact should also be recorded. Increased detriment to the CNS often results from unreported accidents, falls, and the like, not thought important by the patient. Because these accidents may change the misalignment factors of the subluxation, thereby changing the adjustment vectors, they should become known to the practitioner and recorded. An increased shortness of a leg should be viewed with suspicion, and the patient questioned regarding its cause. Occasionally, following trauma, the opposite leg will shorten. This always indicates a change in the adjustment vectors; another misalignment factor of the subluxation has become, because of the trauma, the misalignment that is producing the greatest contracture, affecting the patient’s opposite side. Trauma, in other words, can easily change the subluxation’s misalignment factors, causing a former and previously minor subluxation factor to become predominant in its effects on the reticular formation of the brain stem, causing a loss of the neurological inhibitory innuences to the extensor musculature on the patient’s opposite side. Such an occurrence signals a red-light to the practitioner, warning him that re-x ray is imperative, a new adjustic vector required. If he fails to heed the red-light and continues on adjusting the patient can relapse, and may develop new symptoms.
Agreement of all methods and devices used to determine imbalance in nervous conduction should be the rule. The leg length check should agree with the thermoscope, and, if it does not, the reason should be determined. For every point “break” on the thermoscribe graph, approximately 1/8 inch shortness of the leg should show. Whatever method of measurement is utilized, agreement with the leg-check should occur before a C1 adjustment is given. An adjustment of C1, no matter how perfectly delivered, constitutes trauma if no neurological imbalance is present. This trauma will express itself within a few days in the patient in terms of the short leg, increased symptoms, and neurological detriment.
Not the least value accruing from accurate leg-checking is that it indicates patient progress. Because C1 is a stressor in the body when it is subluxated, it does not contribute to a healthy body; bodily distortions are not signs of health. The proper use and correct understanding of the significance of the leg-check provides a simple and reliable index for the practitioner.
EQUIPMENT
Leg-checking is a more exact process if the proper table is used. Recommended is the Utterback adjusting table. The body piece is about twelve inches in height, which is the best height for the average practitioner. This height allows the practitioner better control of his gravity center when checking legs. The body piece is upholstered for leg-checking – neither too hard nor too soft. The table is of sufficient weight and structure to insure safety for the patient.
PATIENT ALIGNMENT to the MID-SAGITIAL PLANE
The patient is instructed to remove all impediments, such as a man’s pocketbook, from the back pockets of pants, slacks, etc. These articles may cause a false shorting of the leg because they may turn the patient’s pelvic girdle into the transverse plane when he lies on them. He is then asked to sit at the body piece end of the table, facing away from the headpiece. The practitioner guides the patient onto his back, aligning the patient’s spinal column and head to an imaginary line which divides the adjusting table into two equal halves (Figure 1).
The better practice, especially for practitioners who lack experience in leg-checking, is to establish a permanent line midway through the length of the adjusting table (Figure 1). Another line is placed vertically on the wall at the headpiece end of the table. The adjusting table line is then exactly aligned to the vertical line by moving the adjusting table, insuring greater accuracy in sighting the centers of the patient’s head, shoulders, and pelvis to the vertical line and the table center line (Figure 2).
If the patient is tall, his legs may extend beyond the end of the body piece to the extent that his knees may bend. If this occurs, an additional support of the same height as the table’s body piece should be used. The patient’s feet and ankles, however, should extend beyond the body piece, providing additional support to permit grasping the shoes and performing the leg-check. (Fig. 2)
The practitioner checks the patient’s position on the table. The glabella, the center of the chin, episternal notch, and pubic center should lie directly above the table center line. This procedure insures that the patient is centered to the mid-sagittal plane (Fig. 2).
Figure 3 shows an incorrect placement of the patient on the table. The head is turned in the transverse plane, and neither the glabella nor the center of the chin aligns to the mid-sagittal plane. A comparison of the legs to the table’s center line quickly shows that the patient’s legs do not parallel the line. This error in placement could cause a false leg shortening.
After checking the patient’s position in relation to the table’s center line, the practitioner slightly raises each of the patient’s legs, one at a time, and places them in parallel alignment to the table’s center line. The legs are not dragged across the table top as this error will falsely shorten a leg. Dragging a leg against the table top pulls the musculature on the posterior surface of the patient’s leg, producing the error.
ALIGNMENT TO THE PATIENT’S SAGITTAL PLANE
The practitioner aligns his sagittal plane to the patient’s sagittal plane. This procedure assures that lateral displacement of the practitioner’s body will not cause error in leg checking by producing greater shoe pressure from one side of his body. A continuation on the floor of the midcenter line of the adjusting table aids alignment of the two sagittal planes (Fig. 4).
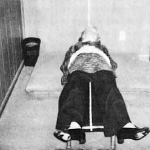
Positioning himself so that his vertical mid-sagittal plane is at right angles to the patient’s horizontal mid-sagittal plane, the practitioner places his feet laterally and equidistant from the extended mid-center line between his feet. His feet are turned out at an approximate 45° angle. The width between the feet is approximately equal to the width of his pelvis.
Bending his knees, the practitioner settles down his thighs along the same plane as described by his feet. He keeps his lumbar spine fairly straight. In bending down, the knees flex more rapidly than the joints of the hips; they “lead the way”, so to speak. The practitioner should not “squat” down with the center of his gravity back so far that he will tend to produce a pulling action when checking the patient’s feet. His body weight should be sufficiently forward so that there is a slight pushing action against the patient’s feet, so that he cannot maintain his position without holding the table for balance. His hip sockets should be slightly higher than his knee sockets. This position permits the necessary forward pressure against the patient’s shoes of approximately 5 lbs. per shoe, and control of the pressure by the practitioner by pushing downward with his knees. This downward pressure brings his body forward. Figure 5 illustrates the correct position from the lateral view, and Figure 6 shows the incorrect posture.
A triangle is formed by the practitioner when he is in the checking position. The apex of the triangle is at the practitioner’s pelvic center of gravity, and the sides of the triangle are formed by the practitioner’s thighs. A line just above the practitioner’s knees represents the base line. This triangle serves the purpose of aligning the practitioner, the base line of the triangle paralleling a line across the heels and shoes of the patient which is at right angles to the patient’s mid-sagittal plane. The triangle, with its apex directly over the mid-center line and its base parallel to the line at right angles to the patient’s sagittal plane line, alerts the practitioner if his body is rotated in the transverse plane (Fig. 7).
Figure 7 shows that there is a slight rotation of the practitioner’s body. The right knee is farther back of the rule bisecting the mid-center line, or patient’s mid-sagittal plane, than the left knee. A body rotation of this nature would probably cause some shortening of the patient’s right leg because slightly more pressure against the right leg would result. The base line of the triangle and an imaginary line across the patient’s feet would not parallel.
The practitioner should position himself neither too close nor too far from the patient’s feet, as either wrong position can cause error. The base line of the triangle is used as a guide, and the patient’s feet should closely approximate or even touch the base line during the checking process, neither breaking through the triangle’s base line nor being more than two or three inches in front of it.
The distance from the center of each of the practitioner’s knees to the imaginary line across the soles and heels of the patient’s feet should be equal, thereby indicating that the practitioner’s body is not rotated.
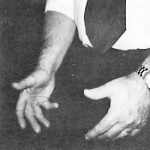
THE ARCIFORM
The practitioner forms his hands in a curved position as illustrated (Figure 8), called the arciform. It is a bow-like shape, and required for holding the patient’s shoes properly. The backstay of the shoe (part of shoe above the heel) rests in the palm of the hand, supporting the foot. The little finger is placed under the heel of the shoe so that sufficient pressure is exerted to keep the heel of the shoe against the patient’s heel. The thumb rests gently along the outside of the shoe, paralleling the patient’s leg.
This method of holding the patient’s shoes allows control of the feet of the patient, and they can be squared to a line bisecting the patient’s mid-sagittal plane at right angles, or parallel to the base line of the triangle. Care must be taken that no downward pressure is placed on the patient’s legs; neither should they be lifted from the table except sufficiently to obtain full extension of the legs.
It is a better procedure to take one of the patient’s shoes at a time and align it to the line bisecting the midsagittal plane of the patient.
The patient’s legs should lie on the table in a relaxed position. The tendency of some patients to assist by tightening their ankle joints or bringing their feet together should be discouraged. If a patient cannot relax either or both of his legs, it may indicate that a subluxation is forming at C-1, which may not yet be apparent in a deficiency of leg length.
Positioned in the checking posture, the practitioner checks his midsagittal plane for alignment at right angles to the patient’s mid-sagittal plane, verifies that the base line of the triangle is parallel to a line across the patient’s soles and heels confirms that equal distance exists from the center of each knee to the line across the patient’s soles and heels, and that he can control his weight forward by pressing down with his knees in order to bring about a 5 pound pressure against the patient’s heels. He then places his fore-arms, elbows slightly outward, across his thighs, somewhat at a 45° angle (Figure 9). Forming his hands into the arciform position, he secures the patient’s shoes, squares them as previously described, pushes downward with his knees to exert the required pressure against the patient’s extensor musculature, rocking slightly forward on the balls of his feet which permits his knees to come downward. If it is necessary to close any little distance between the patient’s feet, the practitioner does so by bringing his knees equally toward each other.
The patient’s shoes are compared in establishing leg deficiency by judging one shoe against the other at that point where the heel of the shoe attaches to the back stay. Shoe heels and soles are often unequally worn and frequently shoes are warped from wear. This is especially true if the patient has been walking in them with a short leg. The unconscious tendency to splay, or turn out, the foot of the short leg causes a twisting motion in walking which increases damage to the shoe on the affected side. Circular markings are often seen on the leather soles of the shoes of patients with a short leg.
EFFECTS of the DURA METER on the SHORT LEG
There are many factors involved in a leg deficiency that are usually reflected in the C1 subluxation. A subluxation, for example, may be just forming, or loss of equilibrium may be occurring at the time of the leg-checking process. Rigidity or tenseness may indicate either of these factors; the patient cannot relax. Sometimes a loss of resistance can be felt by the practitioner if he pushes toward the patient’s body on the tense leg as compared with the opposite leg. These signs are indicative of an on-coming subluxation at C-1.
A more dramatic indication of an on-coming subluxation is observed when the patient’s head is turned either to the right or left while checking for the short-leg. Rotation of the patient’s head may cause one leg to shorten. If so, the disparity is due to a corkscrewing of the dura mater narrowing the cervical canal. Caillet (1964) states: “In rotation of the head, the length of the canal is not influenced, but the cervical canal narrows, not from bony closure but from spiral motion of the dura.”1
The dura mater is attached to the circumference of the foramen magnum and to the posterior surfaces of the second and third cervical vertebrae.2 It is clear, therefore, how rotation of the head will produce a narrowing of the cervical canal. The narrowing of the canal from the twisting of the dura produces an imbalance to the CNS similar to that of a misalignment of C1. Both can cause leg disparity. It is highly significant that when C 1 is not sublimated, and is still balanced that turning the head will not cause a leg deficiency. The ANATOMETER despite the greatly increased gravity stress on the spinal column in the erect position, will also show increased readings when the twisted dura increases the narrowing of the cervical canal in cases where an impending subluxation of C1 is forming.
It should be noted further that it is frequently observed when turning the subluxated patient’s head to one side that a lengthening of the short leg occurs. Turning the head to the opposite side may shorten the leg more than in the straight head position. Apparently, in the first instance, the dura effect temporarily relieves the C1 subluxation. In the second instance, it increases the C1 subluxation.
CONCLUSION
The supine leg-check, properly executed, is one of the conclusive tools in determining the presence or absence of C1 neurological insult. It also has a predictable value in ascertaining if a C1 subluxation is forming. By its precise use, the practitioner protects the patient against indiscriminate and needless adjusting, thus preventing relapses in the progress of the patient and future problems for the practitioner. The supine leg-check alerts the practitioner of un-reported injuries, protecting both the patient and the practitioner against serious changes in the misalignment factors of the C1 subluxation that would cause changes in the adjustic vectors. It must, however, be borne in mind that it is only one means of determining the presence of a C1 subluxation, a subjective one at that; and should be used in conjunction and in agreement with other subluxation determining devices.
REFERENCES:
1. Caillet, R. Neck and Arm Pain. F.A. Davis Co. Philadelphia. (p. 27).
2. Gray’s Anatomy, 35th British Ed., W.B. Saunders Co. Philadelphia (1975) (p. 989)